Treace Medical Concepts
A step ahead as the Leader in
3D bunion correction®
Latest Innovations
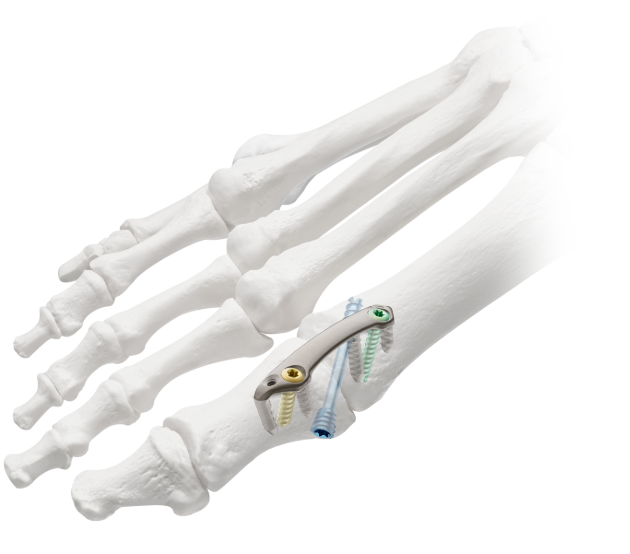
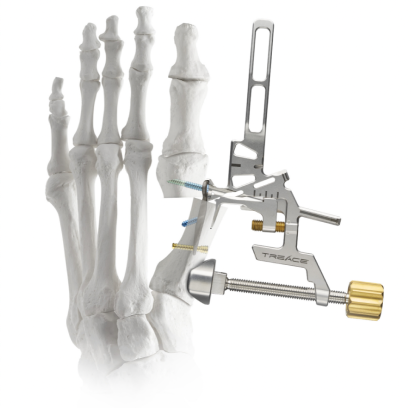
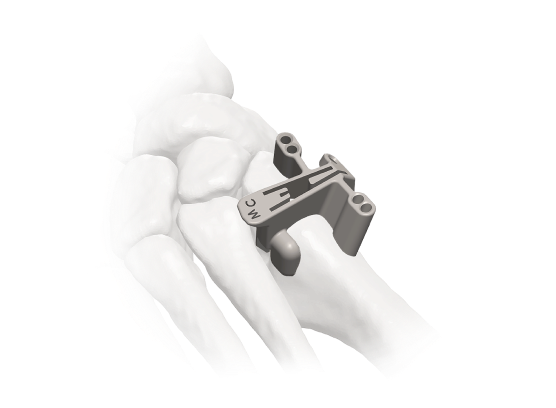

Proven Technology

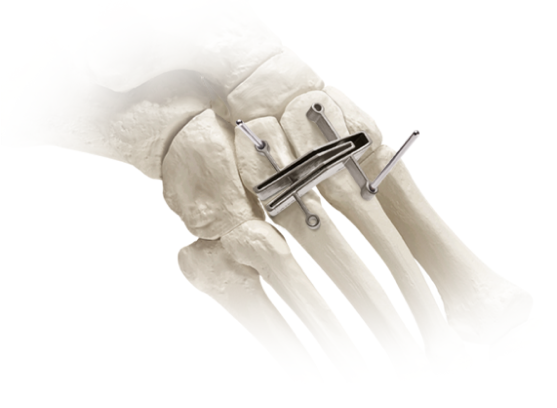

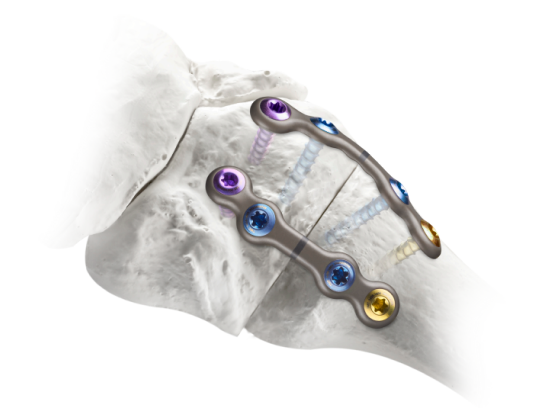
Plating Systems
Next-generation anatomic implants designed to accommodate the 3D anatomy of the tarsometatarsal joint
Learn MoreMinimally Invasive Systems
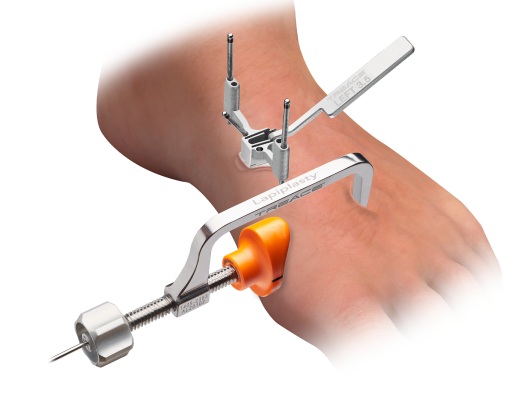
Micro-Lapiplasty®
SpeedPlate™ technology enables the Lapiplasty® procedure through a 2‑cm incision
Learn More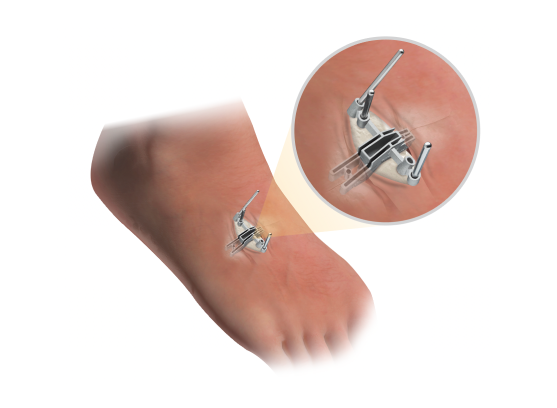
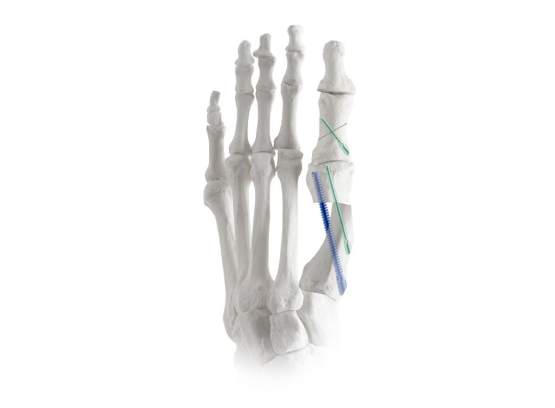
Mini-Adductoplasty™
Specialized incision and cut guides enable the Adductoplasty® procedure through a 4‑cm incision
Learn More
Proven Clinical Outcomes
Lapiplasty® 3D Bunion Correction® has spearheaded the future of bunion surgery
100,000+
100,000 Lapiplasty® procedures performed, including many highly active patients*
24 publications
24 clinical publications directly support the Lapiplasty® procedure
<2 weeks
<2 weeks for patients to return to weight-bearing in a walking boot1,2
97%-99%
97%-99% of Lapiplasty® patients maintained their 3D bunion correction at 13 and 17 months, respectively1,3
Education & Resources
Surgeon Experiences
The opinions expressed by these doctors are not necessarily those of Treace Medical Concepts, Inc.
*TMC, Data on File
M3322E
1. Ray J, et al. Foot Ankle Int. 2019 Aug;40(8):955-960.
2. Dayton P, et al. J Foot Ankle Surg. 2019. 58:427-433.
3. Dayton P, et al. J Foot Ankle Surg. 2020, 59(2):291-297.